National Minority Health Month, led by the HHS Office of Minority Health, brings attention to persistent gaps in health outcomes across communities, particularly along racial and ethnic lines. This year’s focus on social drivers of health highlights something important: many of these gaps take shape long before someone seeks care.
Maternal health offers a clear example. Across Florida, outcomes vary significantly by race and ethnicity, pointing to patterns that extend beyond clinical care alone.
So what does that look like?
Maternal Health Disparities Show Up Clearly in the Data
Maternal health disparities are not subtle. They show up clearly in the data and persist over time.
Across Florida, maternal mortality rates have fluctuated over time, with a sharp increase in 2021 before declining in recent years. Even with that improvement, differences across racial and ethnic groups remain evident.
Black or African American women consistently experience higher maternal mortality rates than other groups. In 2023, the rate was 48.5 deaths per 100,000 live births, compared to 12.0 among White women and 11.9 among Hispanic or Latino women. These gaps widened sharply in 2021 and, while they have narrowed since, they have not disappeared.
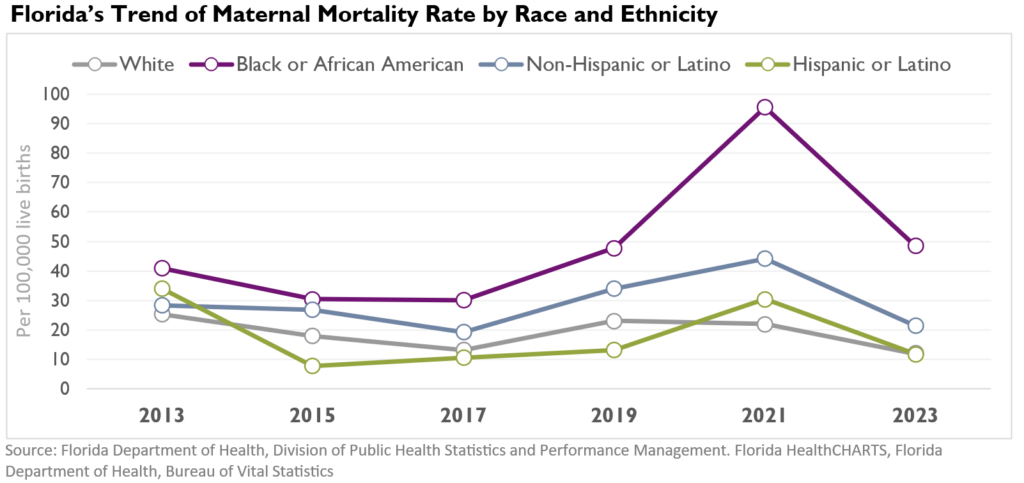
These differences are not isolated. They appear over time and point to differences in the conditions leading up to care, which shape health long before a clinical visit.
Disparities Reflect Differences That Build Over Time
Maternal health disparities do not emerge from a single moment. They build over time.
Across Florida, Black or African American women continue to experience the highest maternal mortality rates, even as overall rates shift.
Severe maternal morbidity, or serious complications during labor and delivery, also varies across populations, with higher rates among Black or African American women and increases across all groups.
These patterns are not driven by one factor. They are consistent with differences in underlying health, access to care, and broader social and economic conditions, often described as social drivers of health. This is where maternal health disparities take root.
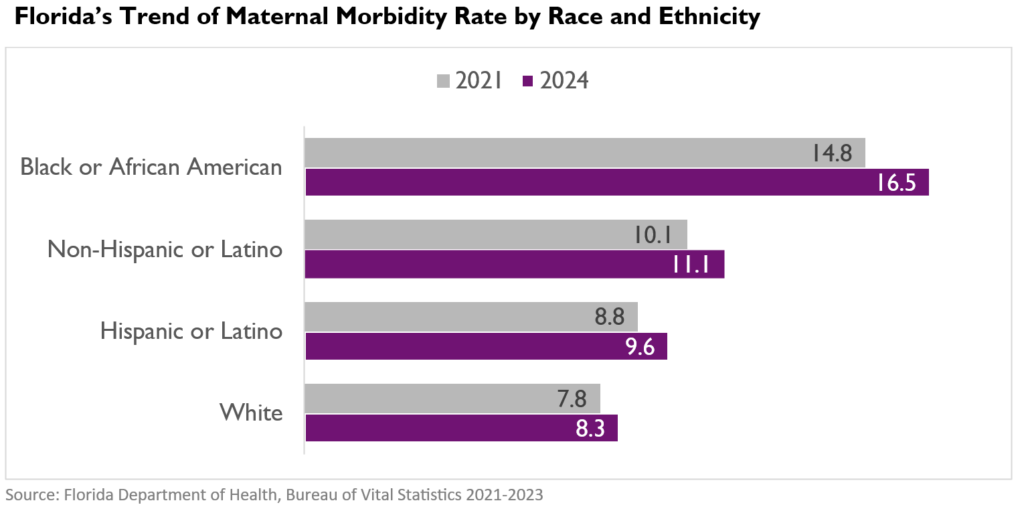
Maternal Health Disparities Don’t Start in the Doctor’s Office
It is easy to focus on what happens during pregnancy or delivery. But maternal health disparities often begin much earlier.
These patterns are not driven by a single factor. They point to differences in access to care, underlying health conditions, and broader social and economic conditions – often described as social drivers of health – that shape risk over time. Research suggests that multiple factors, including healthcare quality, chronic conditions, and social determinants, contribute to these disparities.
By the time someone reaches care, those factors have already had an impact.
That changes the conversation. It shifts the focus from treatment to prevention. From individual care to community conditions.
Final Thoughts
Maternal health data makes one thing clear: disparities are not created at a single point in time. They develop over months and years, shaped by access, resources, and community conditions.
By the time someone reaches care, much of the story has already been written.
Understanding maternal health disparities means looking beyond clinical care and examining the conditions that shape health over time.
Learn more about how Crescendo approaches this work through our Social Determinants of Health framework, and how it informs our Community Needs Assessments and planning efforts.
